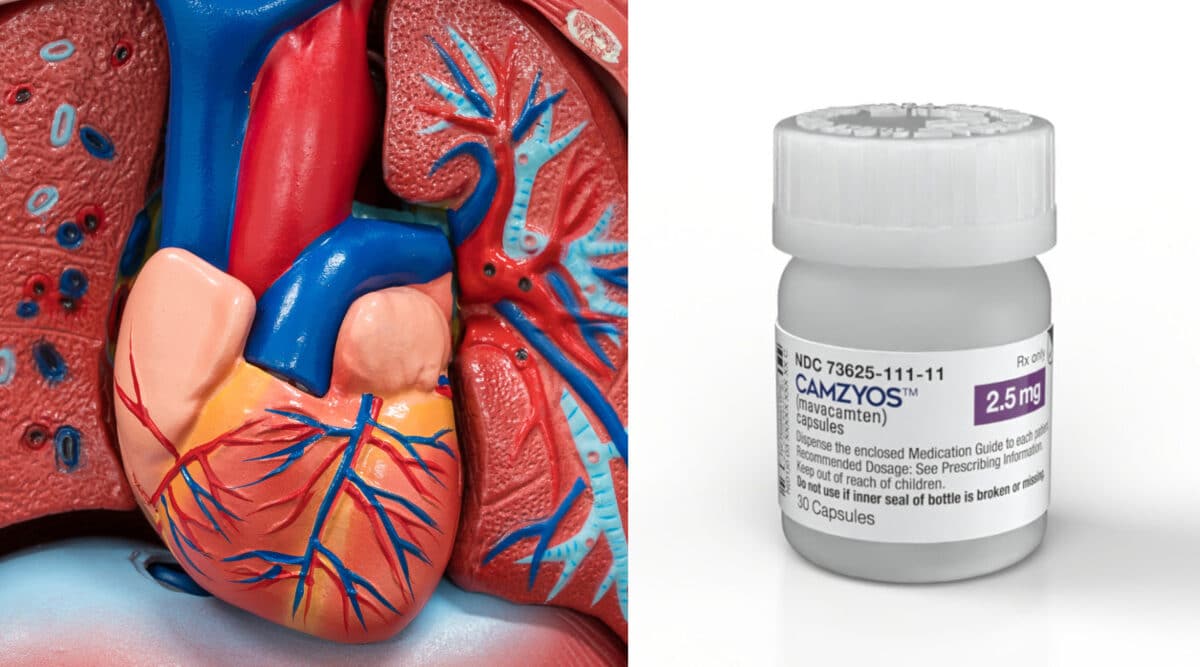
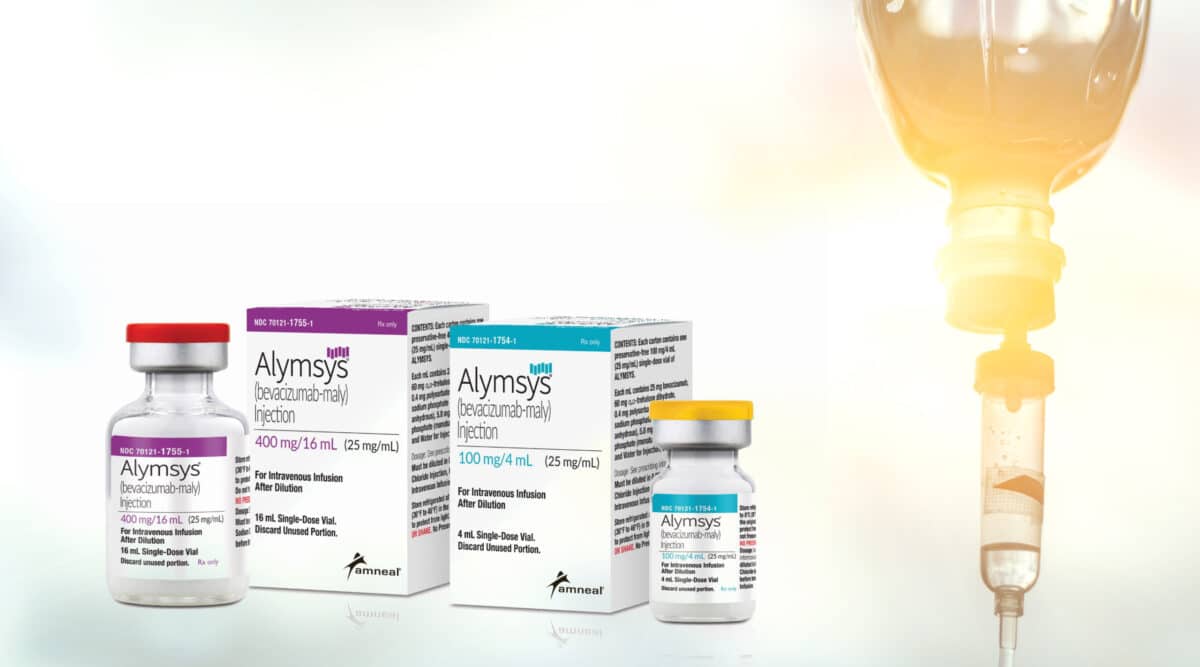
The National Home Infusion Association (NHIA) recently published the results of a survey of patients who had received a home chemotherapy infusion to gauge their level of satisfaction across a number of metrics. The results show that these home infusion patients are very satisfied with services, understand medication instructions, and 89.54% of the patients completed their therapy with only 0.02% adverse reactions related to the administration.
National Home Infusion Association (NHIA) estimates that approximately 132,000+ patients annually received home infusions of chemotherapy agents since 2019 with the trend increasing. Given the criticism of home chemo infusions by hospital-based infusion providers it is not surprising that NHIA would want to ensure that their patients were satisfied with the home infusion experience.
The purpose of this study was to quantify the level of patient satisfaction and to determine any reason for discontinuation from home infusion services. The findings showed a very low rate of discontinuation with more than 90% completing therapy. Of those that did not complete therapy 8+-% died of non-administration-related causes or were hospitalized for non-administration-related causes.
As noted in the published table (click below), patient ratings were very strong in support of home provided services with the majority of metrics in the 90%++ range (strongly agree).
Some deeper evaluation is required related to two outlier results. Question 11, “I was satisfied with the overall quality of the home infusion services provided” dropped precipitously. NHIA points out that when the top two results are combined (Strongly Agree and Mostly Agree) the results increase to 97%. The score in Question 12 – “I would recommend home infusion to family and friends,” similarly suffered but fares much better when the top two options are combined. Future surveys may want to take a deeper dive in these areas to understand patient thinking or rephrasing certain questions.
Several questions relate specifically to the local home infusion company. However, others can be attributable to the specialty pharmacy providing both the therapy and critical services, e.g., authorization and billing (usually worked out before shipment of the drug to the home care company.) For example, in Question 3 patients are asked about delivery of the medication prior to the scheduled appointment. It received the third lowest score and indicates an opportunity for a specialty pharmacy quality improvement assessment.
CLICK HERE to read the full text of the report and VIEW THE TABLE
Chemo at Home: High Rate of Satisfaction, Low Rate of Discontinuation
Overall, 97% of patients said they were satisfied with at-home chemotherapy infusions.
The following article features coverage from the NCCN 2022 Annual Conference.
Receiving chemotherapy infusions at home appears to be safe, and patients reported a high rate of satisfaction, according to research presented at the NCCN 2022 Annual Conference.
Most patients in the study completed at-home chemotherapy as planned, and none of them stopped treatment because of adverse drug reactions.
In a survey, most patients said they understood their medication instructions, were informed about potential side effects, and were satisfied with at-home chemotherapy.
Researchers assessed the safety of home chemotherapy infusions in 153 patients using 3 parameters — treatment completion, adverse drug reactions, and unplanned hospitalizations.
The researchers also surveyed 328 at-home chemotherapy recipients using a 12-question survey developed by the National Home Infusion Association. The survey responses were submitted between 2019 and 2021.
The survey used a Likert scale (“strongly agree” to “strongly disagree”), and the following answers are the highest rated option (“strongly agree”).
All patients said the home infusion pump was clean when delivered, and 99% said it worked properly. Most patients said they knew who to call for help (98%), responses to after-hours calls met their needs (86%), and the nurse or pharmacist explained the possible side effects of treatment (91%).
Nearly all patients said they understood the instructions on how to wash their hands (98%), give home infusion medications (97%), care for the IV catheter (97%), store their medications (96%), and use the home infusion pump (98%).
Jen Smith for Journal of National Comprehensive Cancer Network
Simpson MC, Haines DJ. Patient satisfaction and reason for discontinuation of home infusion for cancer patients. Presented at NCCN 2022 Annual Conference; March 31 – April 2, 2022. Abstract HSR22-168.