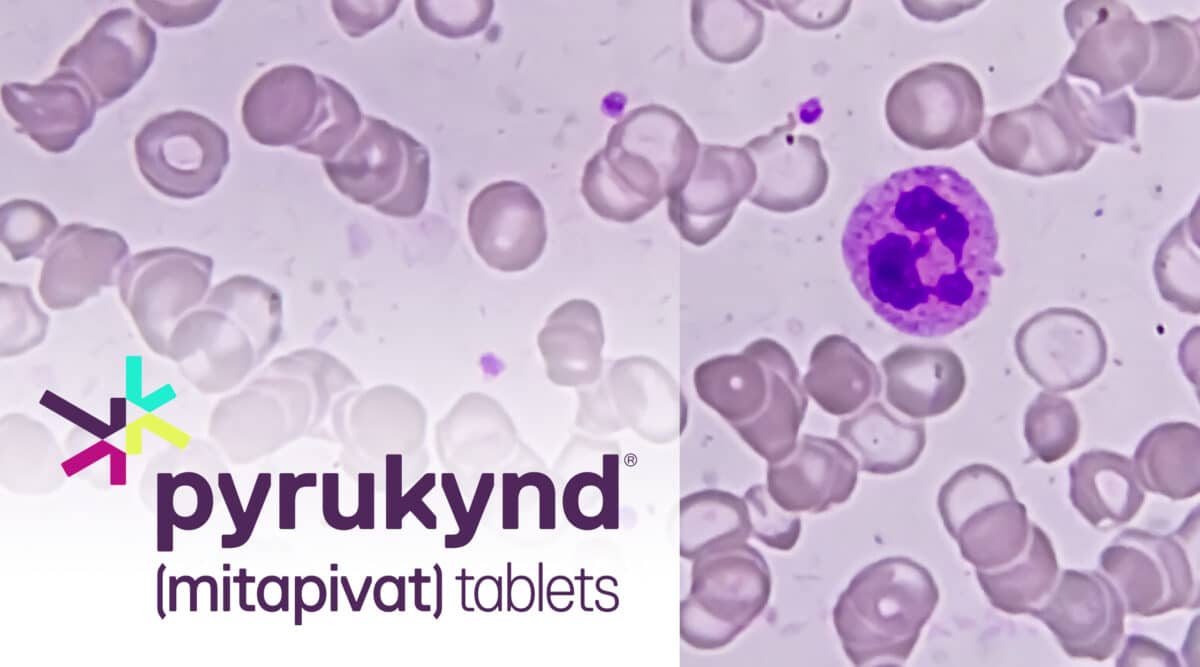
Last week the FDA approved a new oral therapy, Pyrukynd (mitapivat) from Agios Pharma, to treat hemolytic anemia in adults with pyruvate kinase (PK) deficiency. PK is a disorder in which red blood cells are destroyed faster than they can be made.
PK deficiency is rare, with an incidence of three to nine cases per one million people. Best estimates are that PK deficiency affects approximately 3,000 people in the U.S. However, PK deficiency is often misdiagnosed or goes undiagnosed, making it difficult to determine its frequency in the general population.
Pyrukynd became the first FDA-approved medicine for the disorder. It is an inherited disease that can cause lifelong complications including gallstones, pulmonary hypertension, osteoporosis and more. Patients with PK deficiency have a range in severity of symptoms, which include fatigue, unusually pale skin, jaundice (yellowing of skin and eyes), shortness of breath, and a fast heart rate. Patients can also develop an enlarged spleen, too much iron in their blood from repeated blood transfusions, and gallstones (small deposits in the gallbladder or bile ducts).
Pyrukynd must be closely monitored for dose titration from 5 mg up to the maintenance dose of 50 mg over the first 3+ months of therapy.
Pyrukynd will launch at an annual price of $334,880, before insurer’s discounts.
Given its high cost and very small population in the US, it is highly probable that Pyrukynd will be placed into exclusive distribution with a specialty pharmacy.
FDA approves treatment for anemia in adults with rare inherited disorder
February 17, 2022
Action
FDA has approved Pyrukynd (mitapivat) tablets to treat hemolytic anemia (a disorder in which red blood cells are destroyed faster than they can be made) in adults with pyruvate kinase (PK) deficiency.
Disease or Condition
PK deficiency is an inherited disorder that causes premature red blood cell destruction, which leads to anemia (a decreased number of red blood cells).
PK deficiency is rare. In clinical practice, its frequency is approximately three to nine cases per one million people. However, PK deficiency likely is misdiagnosed or undiagnosed, making it difficult to determine its frequency in the general population.
Effectiveness
The effectiveness of Pyrukynd was evaluated in two studies. One was a randomized, double-blind, placebo-controlled clinical study of 80 adults with PK deficiency who did not receive regular blood transfusions. The other was a single-arm study of 27 adults with PK deficiency who received regular blood transfusions. In these studies, patients received Pyrukynd up to 50 mg orally twice daily after an initial dose titration (adjustment) period. Participants received Pyrukynd for an average duration of about 24 weeks in the randomized study and an average duration of about 40 weeks in the single-arm study.
In the randomized study, the effectiveness of Pyrukynd was based upon hemoglobin response defined as a 1.5 g/dL or greater increase in hemoglobin concentration from the beginning of the study that was sustained at two or more scheduled assessments. Hemoglobin is a measure of the amount of red blood cells that are not destroyed. At the end of the study, 40% of participants receiving Pyrukynd had a hemoglobin response compared with no participants receiving placebo.
In the single-arm study, effectiveness was based on reduction in transfusion burden, defined as at least a 33% reduction in the number of red blood cell units transfused during the last 24 weeks of treatment compared with the historical transfusion burden on the individual participant (standardized to 24 weeks). Thirty-three percent of participants who received Pyrukynd met this reduction in transfusion burden, including 22% of participants who did not require any transfusions over the last 24 weeks of treatment.
Safety Information
Because of drug interactions, patients should either avoid using Pyrukynd with certain other medications or adjust the Pyrukynd dose. Abruptly stopping Pyrukynd could worsen premature red blood cell destruction. Patients should avoid suddenly stopping or pausing Pyrukynd and follow their health care provider’s instructions for discontinuing treatment.
The most common side effects of Pyrukynd are decreases in estrone and estradiol (types of the estrogen hormone) in men, increased urate (a type of salt in the body), back pain, and joint stiffness. The effects of Pyrukynd on estrone and estradiol could not be reliably assessed in women because of normal changes in these hormones during the menstrual cycle and use of hormonal contraception.
Designations
This application received orphan drug designation, fast track designation, and priority review.