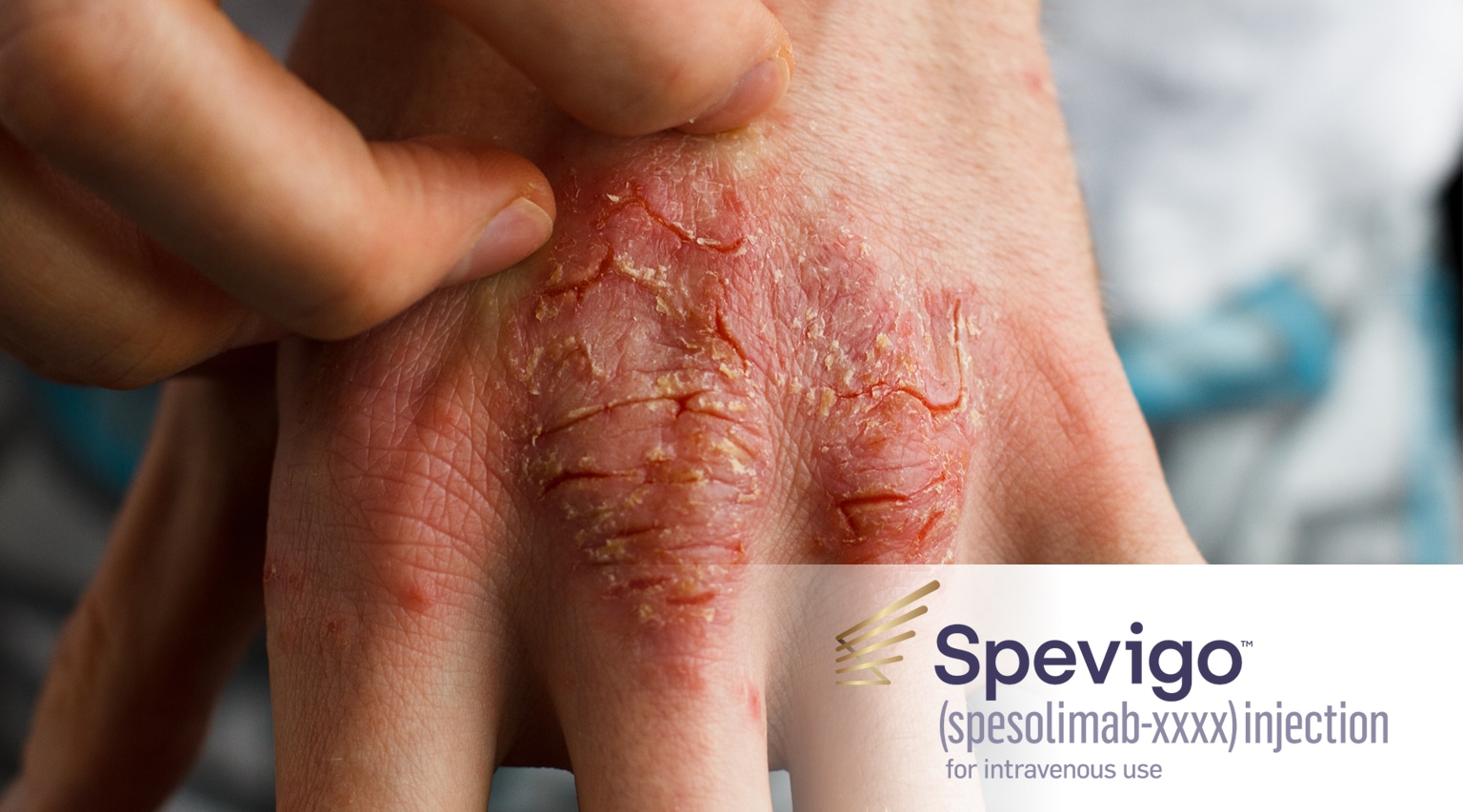
The FDA recently approved a novel infused therapy, Spevigo (spesolimab-sbzo) from Boehringer Ingelheim), with an indication for the treatment of generalized pustular psoriasis (GPP) flares in adults. Unlike virtually all non-gene therapy approvals in the specialty infusion segment, Spevigo is a ‘1 and done’ therapy (although a second dose may be warranted based on patient response.) Efficacy is considered high with 54% of trial participants showing no visible pustules after one dose.
GPP incidence is 1 in 10,000 people in the US. The condition has proven difficult to both diagnose and manage with available therapy. Distinct from plaque psoriasis, GPP is a rare and potentially life-threatening neutrophilic skin disease, which is characterized by flares (episodes of widespread eruptions of painful, sterile pustules all over the body). Severity of GPP flares can vary, but complications such as sepsis and multisystem organ failure can occur. Patients also experience severe quality of life impacts.
Boehringer Ingelheim did not release pricing information at time of approval.
Analysts suggest that the price for the single infusion will ring in at about $58,000.
As a rare condition, with fewer than 30,000 potential patients, it would not be surprising to see this infused therapy launched through a specialty pharmacy distribution model.
———————————————————————————-
FDA Approves Spevigo for Treatment of Generalized Pustular Psoriasis Flares in Adults
Boehringer Ingelheim’s monoclonal antibody inhibits interleukin-36 (IL-36) signaling and is the first treatment specifically approved for this indication.
The FDA approved spesolimab (Spevigo; Boehringer Ingelheim) as treatment for generalized pustular psoriasis (GPP) flares in adults, which marks its first approval by a regulatory authority for this indication.
Spesolimab is a novel, selective antibody that blocks the activation of the interleukin-36 receptor (IL-36R), which is a pathway in the immune system that is involved in the pathogenesis of GPP.
“GPP flares can greatly impact a patient’s life and lead to serious, life-threatening complications,” Mark Lebwohl, MD, Dean for clinical therapeutics at Icahn School of Medicine at Mount Sinai’s Kimberly and Eric J. Waldman Department of Dermatology, New York.
“The approval of spesolimab is a turning point for dermatologists and [physicians]. We now have an FDA-approved treatment that may help make a difference for our patients who, until now, have not had any approved options to help manage GPP flares,” Lebwohl said.
The approval is based on results from the EFFISAYIL (NCT03782792) phase 2 clinical trial, where individuals experiencing a GPP flare were treated with either spesolimab or a placebo for 12 weeks.
At the outset of the trial, most individuals had a high or very high density pustules, and impaired quality of life.
Investigators said that after 1 week, 54% individuals treated with spesolimab showed no visible pustules compared with 6% taking the placebo, investigators said.
Investigators randomly assigned individuals 2 to 1 either a single 900-mg dose of spesolimab or the placebo.
Adverse events (AEs) were reported in 66% of individuals with spesolimab and 56% of those on the placebo after 1 week.
Investigators also reported that 17% and 6% of individuals, respectively, had infections after 1 week.
Serious AEs were reported in 6% of individuals taking spesolimab.
Spesolimab is also under review by other regulatory authorities. It has received breakthrough designation in China, Taiwan, and the United States; priority review in China and the United States; orphan drug designation in Australia, Korea, Switzerland, and the United States; and rare disease designation and fast track in Taiwan, for the treatment of GPP flares.
In October 2021, the European Medicines Agency validated the marketing authorization application, and the submission for spesolimab is under review.